Leaving a cracked tooth untreated isn’t just about looks. It’s actually a structural problem that can seriously mess with your oral health, sometimes a lot faster than you’d think.
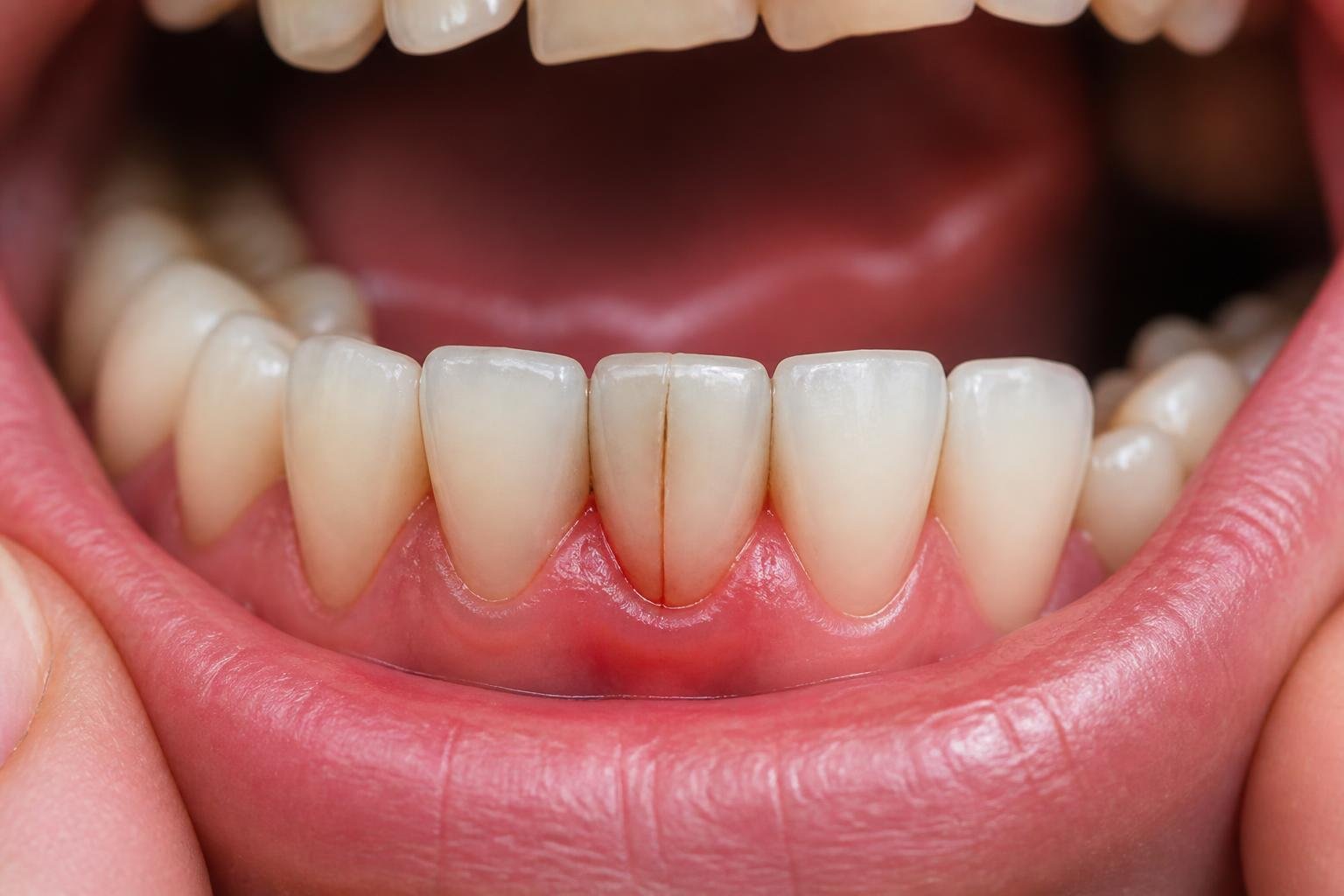
If you’re hoping a cracked tooth might just fix itself, it won’t. Tooth enamel can’t grow back, so once you’ve got a crack, daily chewing and biting will usually make it worse.
Some folks feel sharp pain when they bite or get sensitive to hot and cold stuff. Others don’t notice anything at first. Either way, the risk of infection, nerve damage, and even losing the tooth gets higher the longer you wait.
Key Takeaways
- A cracked tooth won’t heal by itself, and cracks usually get deeper over time.
- Bacteria can sneak into a crack and cause infection or an abscess, which can mean more complicated treatment.
- Getting it treated early, anything from bonding to a crown, gives you the best shot at saving the tooth.
How a Crack Progresses When You Wait
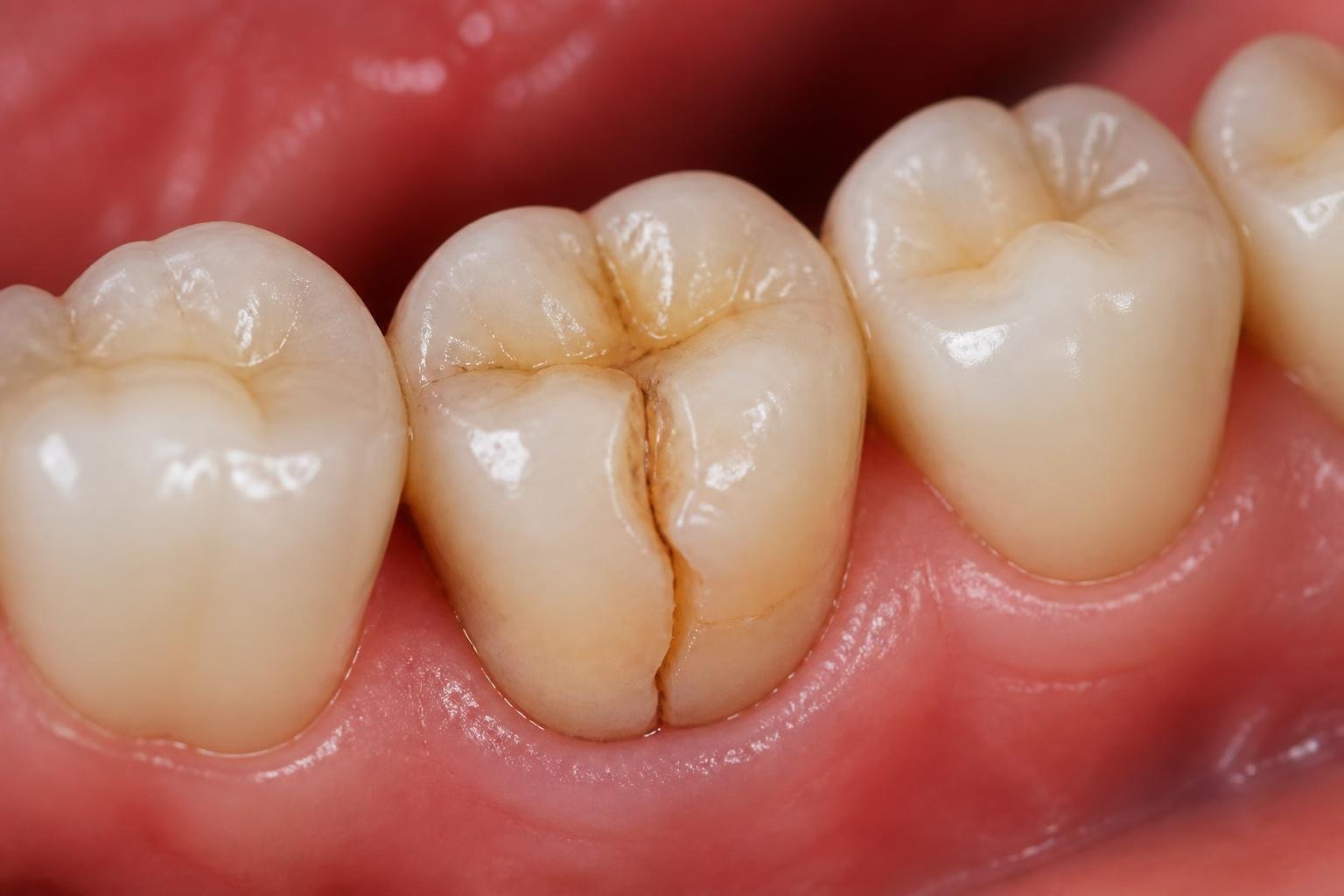
A crack that starts in the outer enamel can work its way into the deeper layers if you ignore it. Things can go from just a little sensitivity to pulp damage, infection, and even losing the tooth.
Why Teeth Don’t Repair Cracks Naturally
Unlike bone, tooth enamel doesn’t have living cells to fix itself. So, once you get a crack, your tooth can’t patch it up on its own.
Biting, chewing, and even temperature changes keep stressing the cracked spot. That extra pressure just makes the crack bigger over time. Even if you don’t feel pain right away, the damage is still happening.
From Intermittent Symptoms to Pulp Damage
At first, you might notice:
- Pain when you bite down or let go
- Sharp pain or sensitivity to hot or cold
- Discomfort that comes and goes
These symptoms usually show up when the crack flexes as you chew. If the crack keeps deepening and reaches the pulp, the nerve can get irritated or inflamed. Dentists call this pulpitis.
Once that happens, toothaches can stick around. You might also feel like the tooth is loose or see swollen gums near the crack.
When an Untreated Crack Turns Into Infection or Tooth Loss
If bacteria get into the pulp through the crack, infection can set in. You might end up with a dental abscess at the root, which causes a lot of pain, swelling, and sometimes even a fever.
If you keep waiting, the infection can spread to nearby teeth, your jawbone, or the soft tissue. Suddenly, what could have been fixed with a dental crown now needs an emergency root canal or extraction.
A tooth that early treatment could’ve saved might end up beyond repair. When that happens, you’re looking at tooth replacement options like a dental implant.
Diagnosis, Crack Types, and Treatment Paths
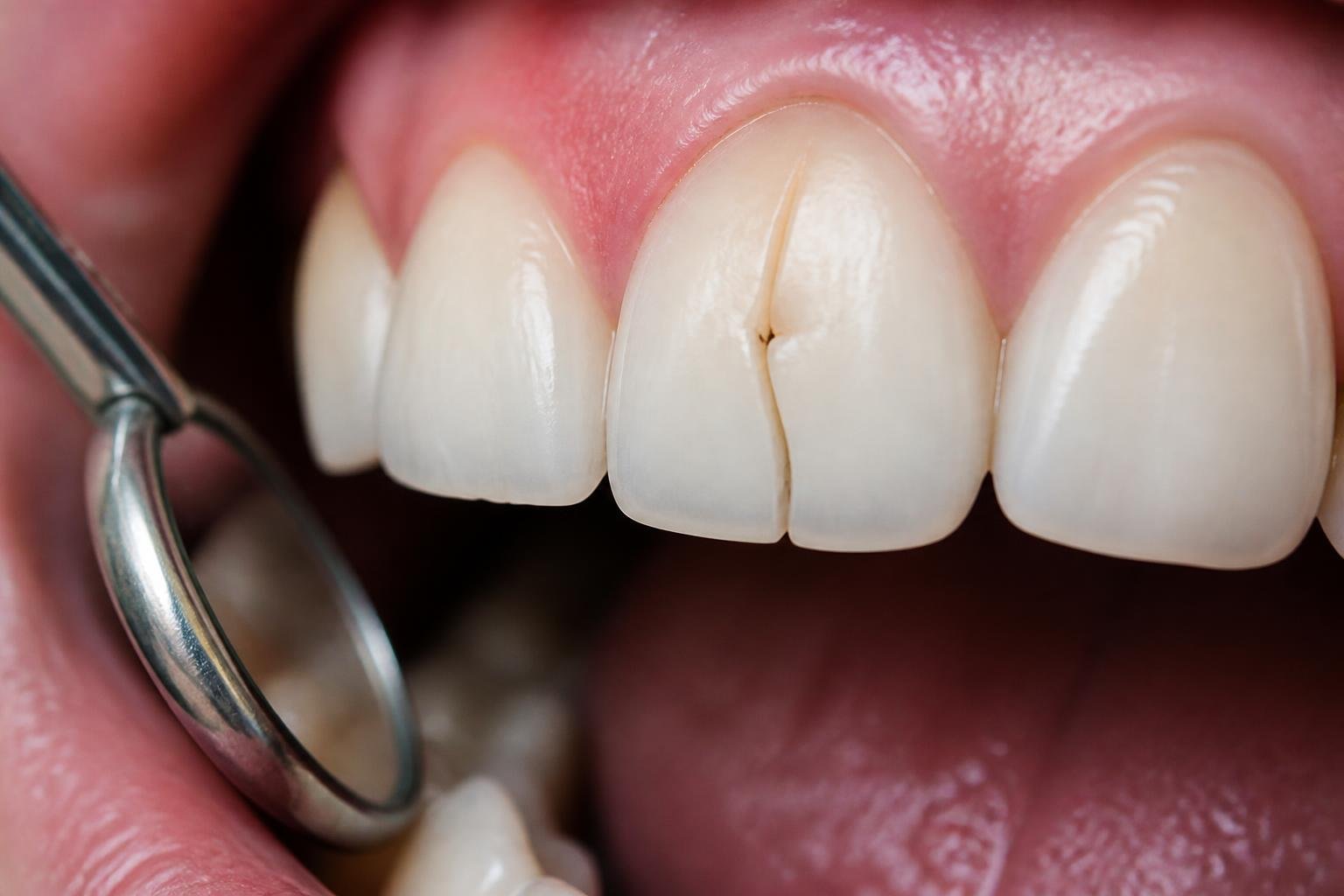
Dentists figure out the right treatment by checking where the crack is, how deep it goes, and if it’s reached the pulp or root. Diagnosis always comes first and shapes everything after.
Types of Tooth Cracks and Why Severity Matters
Not every crack is the same. The type and depth of a crack decide what your options are.
| Crack Type | Description | Typical Severity |
|---|---|---|
| Craze lines | Tiny surface cracks in enamel only | Minor; usually no treatment needed |
| Fractured cusp | A piece of the chewing surface breaks off | Moderate; often treatable with a crown |
| Cracked tooth | Crack extends from crown toward root | Moderate to severe; may need root canal |
| Split tooth | Tooth is divided into two segments | Severe; often requires extraction |
| Vertical root fracture | Crack begins at the root | Severe; often leads to extraction |
Bruxism (teeth grinding) and TMJ problems often cause cracks, especially craze lines and fractured cusps.
How Dentists Diagnose Cracked Teeth
A thorough dental exam is where dentists start. Your dentist will look closely at your tooth, check along the gum line, and ask about your symptoms.
They might also use:
- Dental X-rays or digital X-rays: good for spotting infection or bone loss, but cracks don’t always show up
- Dental dye: helps highlight crack lines on the tooth
- Bite test: you bite on a small stick or tool to see which tooth and direction hurts
- Transillumination: a bright light shines through the tooth to show fracture lines
Treatment Options Based on Depth and Restorability
Treatment depends on how bad the crack is:
- Dental bonding: fills in small surface cracks with tooth-colored resin
- Dental crown: covers the tooth to keep the crack from spreading; common for fractured cusps and moderate cracks
- Root canal therapy: removes infected or damaged pulp if the crack hits the nerve, then covers the tooth with a crown
- Tooth extraction: happens if the crack goes below the gum or splits the root, so the tooth can’t be saved
- Dental implant: replaces the tooth after extraction
If you act early, you’ll usually need simpler and less expensive treatment. Waiting often means more invasive procedures.
Frequently Asked Questions
Can a cracked tooth get worse over time if it isn’t treated?
Definitely. Biting over and over makes the crack deeper, moving from the outer enamel into the dentin and eventually the pulp. What starts as a little surface crack can turn into a split or infected tooth if you wait too long.
What complications can develop if a broken tooth is left untreated for years?
Over time, bacteria can get in and infect the pulp, causing a dental abscess. The infection might spread to the surrounding bone and tissue, and the tooth could end up needing extraction and replacement.
Is it possible for a tooth cracked in half to have no pain, and what does that mean?
Yes, it happens. Some badly cracked teeth don’t hurt, especially if the nerve is already dead. No pain doesn’t mean no problem—the tooth can still get infected and break down even if you don’t feel anything.
Does a cracked tooth always need to be pulled, or can it be saved?
Not every cracked tooth has to be pulled. Dentists can often save minor or moderate cracks with a crown or root canal. Extraction usually only happens if the crack goes into the root or the tooth can’t be fixed.
How can you tell if a tooth is cracked under a crown?
A crack under a crown might make you hurt when you bite, cause sensitivity to hot or cold, or lead to gum swelling nearby. Dentists can check with X-rays, a bite test, and by looking at the gums around the crown for signs of infection or a fracture.
What happens if part of a broken tooth or root is still left in the gums?
If you leave a piece of broken tooth or root in your gums, it can easily lead to infection. Sometimes, you might even get an abscess or notice damage to nearby teeth and bone.
Usually, your dentist will check things out and recommend removing the leftover fragment. This helps prevent more problems down the road.
